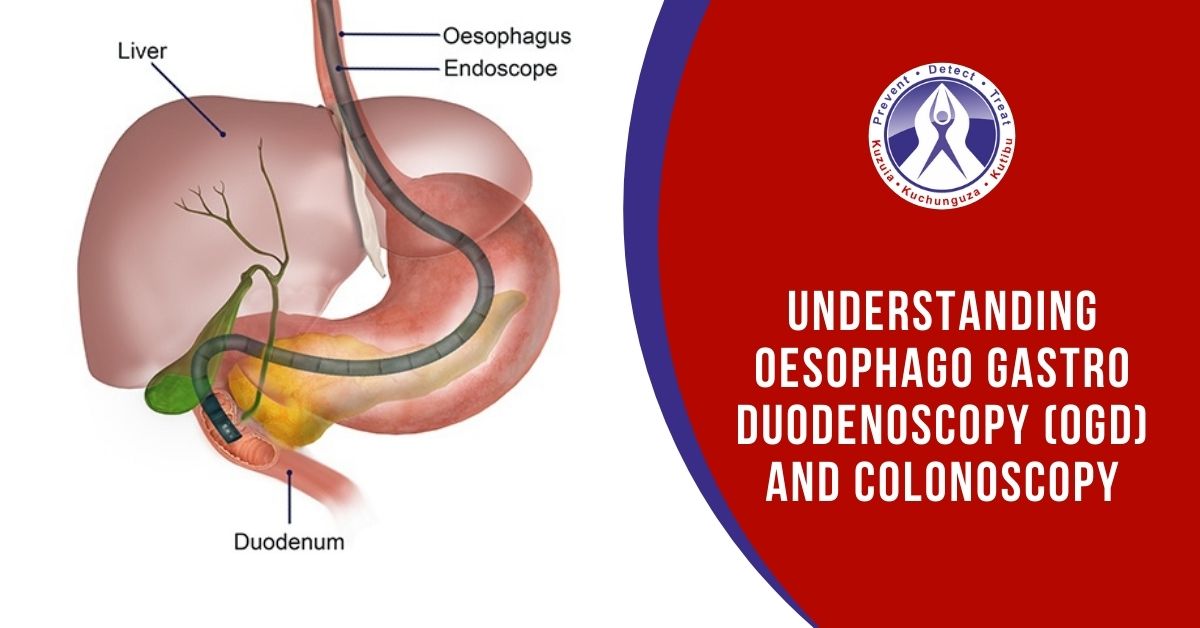
Understanding Oesophago Gastro Duodenoscopy (OGD) and Colonoscopy
4,438 viewsOesophago Gastro Duodenoscopy (OGD) and Colonoscopy are two common types of endoscopic procedures. OGD, also known as Upper GI Endoscopy, is used for diagnosing and treating problems in the upper GI tract. On the other hand, Colonoscopy is used to treat problems in the large intestine and surrounding areas.
Both these procedures are quite similar, particularly because doctors use similar instruments to carry out these procedures. In this blog, we present a detailed yet very simple explanation of an OGD procedure, a colonoscopy procedure, why they are done, and the risks of OGD and colonoscopy.
What is Oesophago-Gastro-Duodenoscopy (OGD) test?
Before we explain what an OGD endoscopy is, you must first understand what an endoscopy is.
Endoscopy is a common procedure that enables doctors to have a direct look at a person’s internal organs. At its core, endoscopy is an imaging procedure as it helps the doctor observe and create detailed images of the organs.
The specialized doctor, called an endoscopist, uses a thin, long tube to carry out an endoscopy. It has a small video camera with a flashlight on one end. Through this video camera, the endoscopist observes and records (live) pictures of a person’s internal organs.
This tube is inserted into the body through an opening, like the mouth or the anus. However, sometimes, the endoscopist might need to do a small incision in the body to insert the tube. It mostly occurs when the organs being tested are difficult to reach via the mouth or anus. But in most cases, no incision is required to perform an endoscopy.
An Oesophago Gastro Duodenoscopy, commonly known as OGD, is an endoscopy procedure that the doctor performs to study the upper digestive system of a person. As the name suggests, OGD involves an examination of the following three gastro-intestinal organs:
Oesophagus – the food pipe
Stomach
Duodenum – the first part of the small intestine
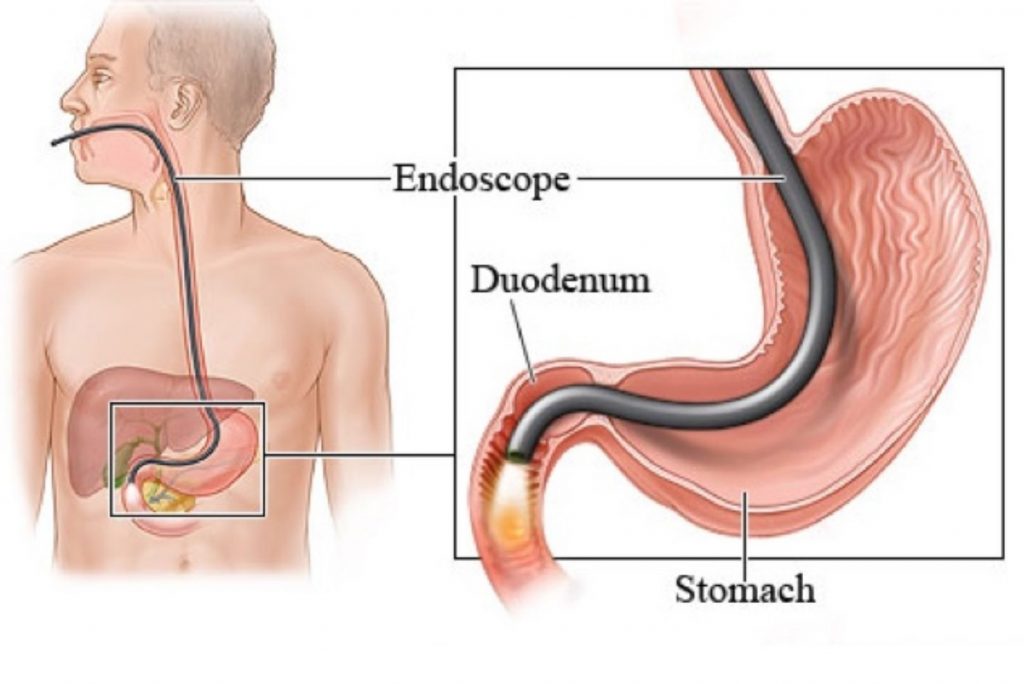
Notably, a more common name of OGD is Upper GI Endoscopy.
When and why doctors conduct an OGD or Upper GI Endoscopy procedure
Your doctor may ask you to undergo an OGD (Upper GI Endoscopy) when you experience some or all of the following symptoms of an unhealthy gut
- Sudden or unexplained weight loss
- Pain in the upper GI tract (Oesophagus, stomach, or duodenum)
- Constant or recurring chest pain or heartburn
- Constant or recurring nausea or vomiting
- Difficulty swallowing food or liquids
- Bleeding in stomach, food pipe, or any part of the upper GI tract
After the onset of these symptoms, your doctor may recommend OGD endoscopy for one or more of the following purposes:
Examine the symptoms
The endoscope enables the doctor to observe internal organs in the upper GI tract closely. That way, they can find out exactly why or how the organs are causing the symptoms.
Diagnose the disease
This close examination of the GI organs also lets the doctor identify if you are suffering from a GI-related disease. In most cases, the doctor will perform a biopsy to diagnose the type of infection or disease present in the tissue. Therefore, OGD endoscopy is a common procedure for diagnosing cancers in the gut like Pancreatic cancer or cancer of the oesophagus.
Treat the symptoms/disease
Ultimately, the goal of OGD or Upper GI Endoscopy is to treat the symptoms or the underlying disease.
Common diseases that doctors have identified through Upper GI endoscopies are gastroesophageal reflux disease (GERD), ulcers in the GI tract, inflammation of one or more GI organs, cancers of the GI tract, precancerous abnormalities, or blockages in the GI tract.
Risks involved in undergoing OGD or Upper GI Endoscopy
Oesophago Gastro Duodenoscopy or Upper GI Endoscopy is a safe procedure and doesn’t cause harmful side-effects in most cases. However, some of the rare complications that some patients may experience are:
- Some patients may experience bleeding in the area from where the doctor takes a tissue sample. This kind of bleeding generally stops by itself and doesn’t require serious medical attention.
- In rare cases, Upper GI Endoscopy may lead to certain kinds of infection in one or more parts of the GI tract. These infections are usually minor and can be treated with antibiotics.
- A serious complication, however, can develop when the endoscope causes a tear in the oesophagus or other parts of the GI tract. This is called a perforation. It requires immediate hospitalization for timely treatment. However, the chances of a perforation occurring during an Upper GI Endoscopy are extremely low.
To reduce the risks of OGD or Upper GI Endoscopy, it’s essential that you understand and follow the instructions given by your doctor thoroughly. For example, your doctor may ask you to fast for around 8 hours before the OGD procedure or not to take some of your medicines on the day of the procedure.
What is a Colonoscopy test and how is it different from Upper GI Endoscopy?
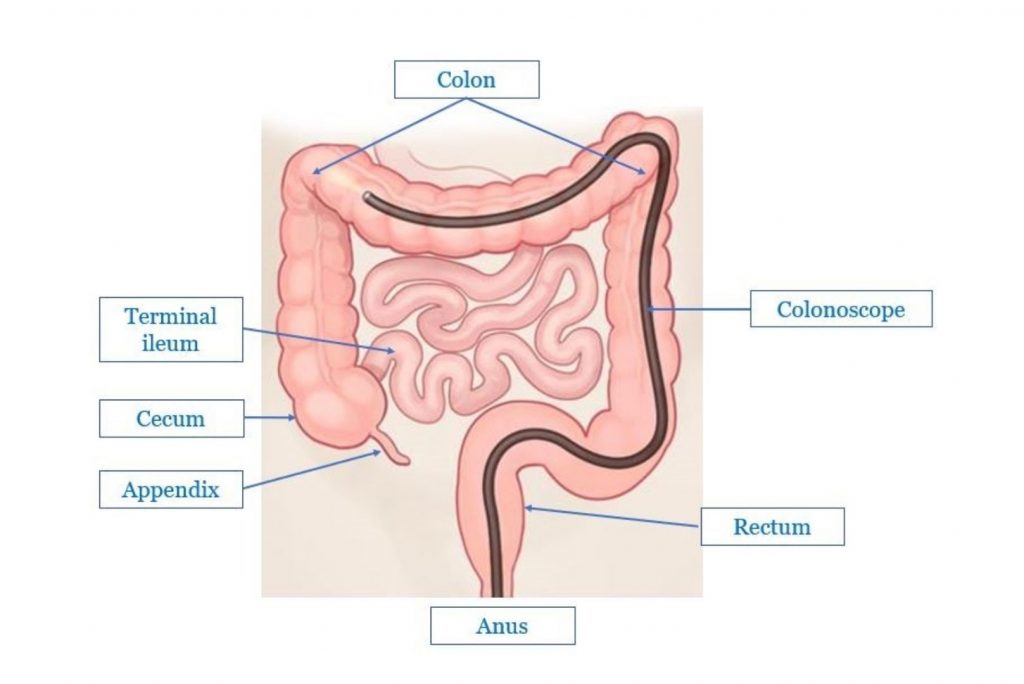
We have already established that doctors use OGD to observe and/or treat the conditions in the upper GI tract. To do the same in the lower areas of the GI tract, doctors use the Colonoscopy procedure.
Doctors use a thin, flexible tube called a colonoscope to perform a colonoscopy. Just like the endoscope, the colonoscope too has a camera and flashlight attached at one end. The doctor inserts a colonoscope through the rectum (anus) of a person and generates live, high definition images of the lower GI organs on a monitor.
The doctor uses colonoscopy to observe the large intestine and related organs, most commonly, the colon and the rectum.
When and why doctors conduct a colonoscopy procedure
Your doctor may ask you to undergo a Colonoscopy procedure when you experience one or more of the following symptoms:
- Chronic abdominal pain
- Sudden or unexplained change in your bowel movements
- Chronic constipation or diarrhea
- Unexplained weight loss
- Bleeding from the rectum
Generally, when a person presents with such symptoms, the doctors want to eliminate the risk of colon cancer. That is why they recommend you undergo a colonoscopy so they can observe and study the conditions that might or might not be cancerous.
Through the colonoscopy procedure, the doctor may attempt to:
Examine the signs and symptoms in the large intestine or the colon area
By having a close look at the intestinal organs, the doctors can know the complexity or severity of these symptoms.
Screen you for colon cancer
To do so, they may use the colonoscope to take a small tissue sample from the affected area and then send it for further examination to declare whether it’s cancerous or non-cancerous.
Look for and treat polyps in the colon
A polyp is a small collection of accumulated cells that lie on the lining of the colon. Although most polyps are harmless, some of them may lead to colon cancer in the future. So it’s vital to treat those in time.
Risks involved in undergoing colonoscopy
Colonoscopy is a safe procedure and doesn’t cause harmful side-effects in most cases. Some of the rare complications of colonoscopy that some patients may experience are:
- Bleeding in the area from where the doctor takes a tissue sample. This kind of bleeding generally stops by itself and doesn’t require serious medical attention.
- Certain kinds of infection in one or more parts of the intestinal organs. These infections are usually minor and can be treated with antibiotics.
- A serious complication, however, can develop when the colonoscope causes a tear in the colon or rectum wall. This is called a perforation. It requires immediate hospitalization for timely treatment. However, the chances of a perforation occurring during a colonoscopy are extremely low.
To reduce the risks of a colonoscopy, it’s essential that you understand and follow the instructions given by your doctor thoroughly. For example, your doctor may ask you to fast for around 8 hours before the colonoscopy procedure or not to take some of your medicines on the day of the procedure.
For OGD or Colonoscopy, Put Your Trust Only in The Experts
Both Oesophago Gastro Duodenoscopy and Colonoscopy are vital procedures that help patients diagnose and treat the early signs of serious diseases like GI cancers, colon cancer, polyps, Gi blockages, and more. It’s, therefore, vital that you consult with doctors that have significant experience in these procedures.
With ultra-modern infrastructure and a trusted team of expert doctors, Regency Medical Centre is the best Endoscopy center in Dar es Salam. We prioritize the accessibility and convenience of the patients over everything else. So over the last 22 years, our team has been consistently working harder to provide the best medical care to the citizens of Tanzania at highly affordable prices.
If you experience any symptoms of abnormalities in the upper GI tract or lower intestinal areas, consult with a doctor at once. Regency Medical Centre provides all the major types of Endoscopic procedures to all Tanzanian citizens on an equitable basis.
To speak to our team regarding endoscopy, book an appointment today.